|
 |
- Search
| Healthc Inform Res > Volume 28(2); 2022 > Article |
|
Abstract
Objectives
Given the challenge of limiting the transmission of coronavirus disease 2019 while simultaneously continuing to provide medical care for other chronic and degenerative diseases and monitor therapy, a remote medical advice and guidance program was created to help individuals receive health services at their homes.
Methods
A descriptive, cross-sectional, and observational study was performed from April 13, 2020 to April 19, 2021 among Petroleos Mexicanos (PEMEX) health services beneficiaries. Mobile text messages were used to assign patients throughout Mexico to a doctor, who coordinated a video call with the nursing service for advice and remote care.
Results
In total, 17,472 calls were registered, with an average duration of 10.28 minutes. Almost half (49.4%) of the people who requested attention through the remote program were workers, 31.5% were workers’ relatives, and 19.1% were retired workers. The average age of the program users was 50.66 ± 18.02 years. A total of 144 doctors from 28 different specialties participated. In this program, 7,163 calls were made because of respiratory symptoms, 1,514 for therapeutic monitoring (prescriptions), and 8,183 because of other diseases, including mental health.
Conclusions
Remote healthcare programs have shown the potential to support the health system. This program is the first to deploy real-time video calls with a health team utilizing institutional electronic clinical records in Mexico. The implementation of this pandemic management program impacted the number of consultations given remotely, resulting in effective triage.
The development of protocols for the prompt management of people with respiratory symptoms caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has been challenging for healthcare systems across the world [1]. The rapid spread of coronavirus disease 2019 (COVID-19) challenged the capacity of health systems to provide care for citizens, generating tensions among health professionals [2]. Facing this double challenge of limiting the transmission of COVID-19 while continuing to provide medical care for other chronic and degenerative diseases and monitor therapy, new strategies have been explored to achieve this goal, as well as to prevent and control the transmission of SARS-CoV-2 [3].
In this regard, remote medical advice and guidance have been considered integral methods for prioritizing medical attention. The first principle of health personnel has been to maintain a focus on the patient while preventing COVID-19 transmission by offering telephone and videoconference services for specialized attention 24 hours a day, 7 days a week [4]. Although it is well known that remote healthcare protocols reduce the risk of infection by diminishing the exposure of health workers and the general population, without compromising patient satisfaction and safety, few studies on this issue have been conducted [5–8].
In Mexico, the promotion and implementation of information and communication technologies (ICT) along with traditional practices of healthcare began in 2004 with the creation of the National Center of Health Technology Excellence, which is the autonomous guiding body for the assessment and management of health-related technologies in Mexico’s national health system [9]. In 2015, it started regulating remote medical services to establish the procedures that health workers who provide these services must follow and the characteristics that establishments offering such services must have, in order to guarantee the highest standard of practice through the use of ICT [10]. Nevertheless, before the COVID-19 pandemic, it was difficult to consider expanding the use of remote medical services due to Mexico’s demographic and economic profile [11].
In 2016, the health services of the state enterprise Petroleos Mexicanos (PEMEX) implemented telemedicine, following the proposal made by the World Health Organization in 1998 to reduce health inequalities in the population and to expand access to quality medical services [12]. As the COVID-19 health emergency developed, the need for remote medical services became clear. In response to the increasing demand, a remote medical advice and guidance program was created to bring health services and advice closer to workers, retired workers, and relatives, to offer them clinical monitoring for chronic diseases and therapeutic monitoring, and to develop educational and health promotion interventions without requiring patients to leave their home. The purpose of this study was to describe this remote medical services program and its role in ensuring the continuity of healthcare during the COVID-19 pandemic.
A descriptive, cross-sectional, and observational study was performed from April 13, 2020 to April 19, 2021 among the workers and retired workers of PEMEX and their families (beneficiaries) who participated in the program.
Health team of the remote health program is “PEMEX closer to YOU.” The health team that oversaw the program was composed of a health coordinator (doctor in charge of coordinating the telephone lines enabled for the remote program), specialist doctors, and personnel responsible for receiving requests and categorizing reasons for clients. calls. A remote monitoring platform was operated by a general doctor, a specialist doctor, and nursing personnel.
The healthcare personnel who participated in the program were health or nursing workers among the at-risk population, according to the criteria issued by the Mexican government together with the Health Secretariat [13], who could not engage in on-site work in the context of the COVID-19 pandemic due to their risk factors (comorbidities).
Starting on April 13, 2020, three mobile phone numbers were made available to 750,000 PEMEX beneficiaries for requesting remote health advice or guidance. This information was disseminated through the official digital media of PEMEX. Patients requested remote visits by sending a text message containing their identification data, such as name and membership number, to mobile numbers that were available 24 hours a day, 7 days a week.
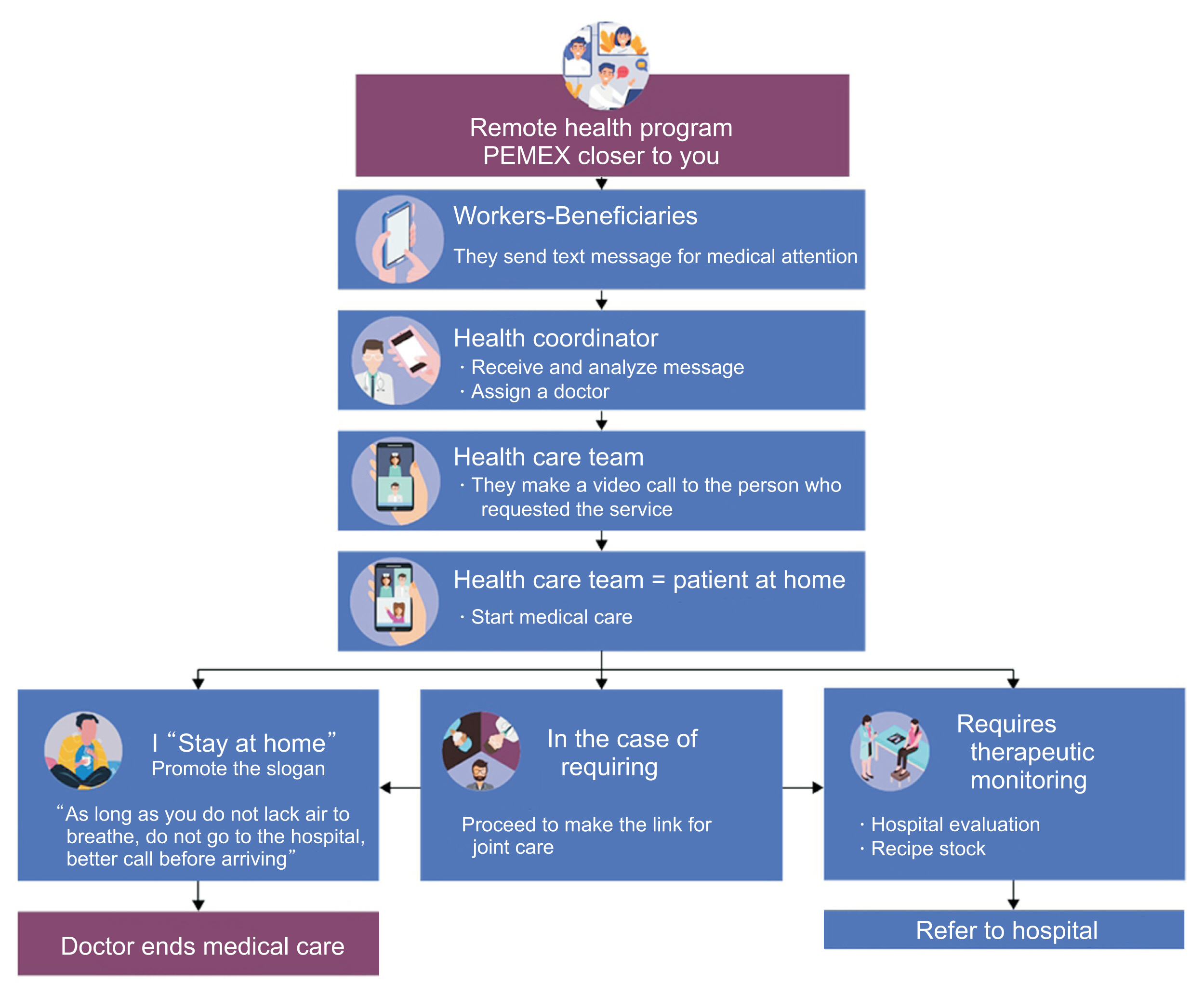
Each message was then received by the health coordinator, who assigned a general doctor and specialist to give advice and remote care. The assigned doctor coordinated with the nursing service to make a video call using an instant messaging app with end-to-end encryption to guarantee the privacy of the tripartite video call with the patient (Figure 1).
If the patient required attention at a hospital, the assigned health team communicated to the liaison of the closest hospital for timely referral and on-site engagement. If the patient showed respiratory symptoms, the assigned health team administered a questionnaire eliciting information about alarming signs, as described in the “Operational guide for contingency care for COVID-19 in Medical Units of Petróleos Mexicanos” [14]. They then decided whether the patient should continue to be monitored at home or seek care at a hospital.
A database was created that contained data on the health personnel who participated in the remote health program throughout Mexico, as well as medical linkage information on hospitals that participated in the program for on-site appointments of the referred patients.
The doctor assigned to each video call registered the appointment on the electronic platform created for the “PEMEX closer to YOU” program. Furthermore, the institutional medical record, known as the Integral System of Hospital Management (Sistema Integral de Administración Hospitalaria [SIAH]), accurately recorded the visit and patient monitoring, with photographic evidence of each consultation offered through the program. The registered data contained the name and specialty of the assigned doctor, the name of the assigned nursing worker, the date and duration of the call, the category of the patient (worker, retired worker, or relative), the affiliated hospital, the state, the reason for the call, whether a specialist doctor was required, whether COVID-19 was suspected, and the conclusion of the healthcare encounter.
The study was approved by the Research Ethics Committee of the Hospital Central Sur de Alta Especialidad (IRB No. CEI-HCSAE-11-20, CI-HCSAE-11-20). Consent was not obtained, as the study was based on registry information.
Information was captured and analyzed in Microsoft Excel and Prisma 9 (GraphPad, San Diego, CA, USA). In a descriptive statistical analysis, central tendency and dispersion measures were determined, along with frequencies and percentages. A choropleth map (used to represent data through various shading patterns or symbols on predetermined geographic areas) was also made to highlight the states with the most significant activity on the remote health program.
Data from April 13, 2020 to April 19, 2021 were assessed. During this period, 17,472 calls were registered. The average duration of the calls was 10 minutes 28 seconds. The majority (56.01%) of the patients were female (9,785) and 43.99% were male (7,687), with a female-to-male ratio of 1.22 to 1. Furthermore, 49.4% of the people who requested attention through the “PEMEX closer to YOU” program were workers, 31.5% were workers’ relatives, and 19.1% were retired workers. The average age of the clients was 50.66 ± 18.02 years.
In this program, 144 doctors from 28 different specialties offered general healthcare. Doctors from the following five specialties answered 80.31% of the total calls (14,031): general doctors (n = 85; 59%), who responded to 10,048 calls (57.51%); dermatologists (n = 2), who answered 7.39% of the calls (1,292); pediatricians (n = 5), who answered 5.84% of the calls (1,020); and anesthesiologists and internists (n = 7 each), who answered 851 (4.87%) and 820 (4.69%) calls, respectively. Table 1 presents information on the doctors who answered the remaining 19.69% of the calls.
Slightly over half (53.94%) of the participating doctors were women, while 46.15% were men. Furthermore, 95 nurses, all women, assisted the doctors during 78.1% of the calls. The ratio of general practitioners to specialists was 1.44 to 1.
Veracruz was the state in Mexico that presented the highest number of remote consultations, with 4,729 beneficiaries who requested remote advice or guidance; followed by Mexico City (4,625 calls), Tabasco (2,977 calls), Campeche (893 calls), the State of Mexico (455 calls), Guanajuato (350 calls), Nuevo León (330 calls), and Yucatán (308 calls), while Hidalgo was the state with the smallest number of calls (248 calls) (Figure 2).
Regarding the reason for the calls, 7,163 calls were requested because of respiratory symptoms, 1,514 for therapeutic monitoring (refill of prescriptions), and 8,183 for other disorders, including mental health. For technical reasons, 612 calls were not concluded.
During the course of the COVID-19 pandemic, important variables were added to the data collection tool to address risk factors for COVID-19 [15], such as diabetes, obesity, and hypertension (Table 2). Information was also collected on whether the patient’s disease required hospital attention or the consultation could be concluded remotely (Table 3). This gap in data collection is shown in our results in the “unregistered” columns.
More than a year after the beginning of the COVID-19 pandemic, the pressure on the health system continues [16]. Remote healthcare programs have shown the potential to support health systems in this context, particularly in low-and middle-income countries, as a way to improve access to healthcare [17]. Nevertheless, problems in the establishment of effective programs using ICT have been a constant and recurring challenge [18].
The implementation of this program makes evident the value of rapid responses of health services through the adequate use of ICT [19]. In several Latin American countries, it is still difficult to find previously reported evidence on the use of ICT for remote healthcare. Nevertheless, in 2016, only 11.8% of general practitioners in the United States [20] worked in a practice that utilized ICT for patient care. Since June 2020, this number has shown exponential growth [21].
In 2016, PEMEX implemented an operational guide for teleconsultation services, becoming a pioneer in the implementation of these technologies, as well as electronic medical records in hospitals. With personnel sufficiently qualified to implement ICT in the health system, this program enabled the rapid adoption of ICT for remote primary medical services during the COVID-19 pandemic [14].
This program was launched to support the beneficiaries of PEMEX, an oil company, and to utilize the expertise of health workers who were at risk for COVID-19 and who could not continue with on-site appointments [13,21]. This allowed the participation of almost 150 doctors. In addition to general practitioners and specialists, nursing personnel offered their knowledge and support. The aim was to optimize the utilization of human resources by implementing an innovative program that used existing personnel in the context of an emerging viral disease that impacted health services worldwide.
There were regional differences in the number of consultations. The average time of the consultations was approximately 10 minutes. Since the calls were focused on taking a clinical history, providing guidance, and referring patients for further care, if necessary, if time is used as a quality indicator, the program achieved adequate standards [22,23]. Studies have suggested that the on-site consultations should have a duration of approximately 20 minutes to satisfy users and comply with quality standards [24,25]. Nevertheless, in telemedicine programs, a standard has not been established for the time required for an adequate consultation, and the duration depends strongly on the reason for the consultation. Previous studies have shown that teleconsultations take on average 10 to 15 minutes to discuss the case and its management [26].
The number of calls received through the program for prescription refills reflects the program’s success by avoiding the necessity for patients requiring monthly follow-up for chronic and degenerative diseases to make in-person visits to refill their prescriptions. This decreased the risk of infection without compromising their treatment for their pre-existing conditions. Furthermore, the records of patients suspected of having COVID-19 enabled the real-time development of strategies for focusing attention on these patients. This allowed the PEMEX health system to implement monitoring programs to optimize resources, without requiring patients to make in-person visits.
The rapid implementation of this remote program could have been challenging for our target population in terms of their capabilities and attitudes due to the lack of adequate equipment, insufficient knowledge of how to use the platforms or mobile equipment, and mistrust of services that do not include on-site attention.
This program is the first to make real-time records of video calls performed with the health team and institutional electronic clinical forms, which provide information about the consultation, the diagnosis, and the resolution of the remote encounter. This result is relevant in the context of the COVID-19 pandemic due to the importance of monitoring chronic diseases.
It is essential to note that no legislation regulates ICT use in health systems in Mexico, which could be a limitation of the development and implementation of ICT systems. In Latin America, the COVID-19 pandemic caused efforts to regularize the policies focused on e-health to grow by leaps and bounds. Together with the National Commission on Sanitary Risks and private entities in Mexico, the National Center of Health Technology Excellence has launched the development of guidelines to regulate this field.
According to the guideline for measuring the maturity level of health institutions to implement telemedicine services published recently by World Health Organization and Pan American Health Organization, the program implemented by PEMEX’s health services can be classified as level 4 [27]. This means that it has an optimal level of consolidation for the implementation of telemedicine services.
The limitations of the study are that the program presented in this study was launched in response to the demand for medical care resulting from the COVID-19 pandemic. As a result of the increase in medical care required for COVID-19 patients, during the development of the program, the information obtained was used to implement improvements and have a greater impact on remote medical care. This explains the lack of data at the beginning of the program, as the demand for care was increasing due to the emergence of SARS-CoV-2, and there was insufficient information for proper planning at the outset. There was also a lack of uniformity in data collection during the registration period due to the high demand for the service. Unfortunately, despite previous experience with telemedicine and remote care programs, there is still much to learn about the use of these tools and the implementation of public policies in developing countries.
In conclusion, the implementation of a remote health program had an impact on the number of consultations given remotely, and proved useful as triage for the appropriate selection of patients who should be seen at a hospital, while giving timely attention to patients who did not need to present to a hospital and those suspected of having COVID-19.
The design and implementation of the “PEMEX closer to YOU” program was a massive effort led by health and administrative personnel, which translated to a substantial number of consultations, thereby establishing the foundations for telemedicine while also contributing to the management of a nationwide health emergency.
Acknowledgments
In memory of Dr. Armando Mejía Nava, coordinator of the “PEMEX closer to YOU” program, who led the logistic coordination of the program, a clear example of leadership, humanism, professionality, and perseverance, whom we will always fondly remember. We are grateful for the participation of César Israel Ramírez Cuervo for the design of the illustrations and the team of the Instituto Politécnico Nacional for supporting us in the statistical analysis and all the health staff that made this program possible.
Figure 2
Map of Mexico showing the geographic distribution of requests for attention through the remote health program.
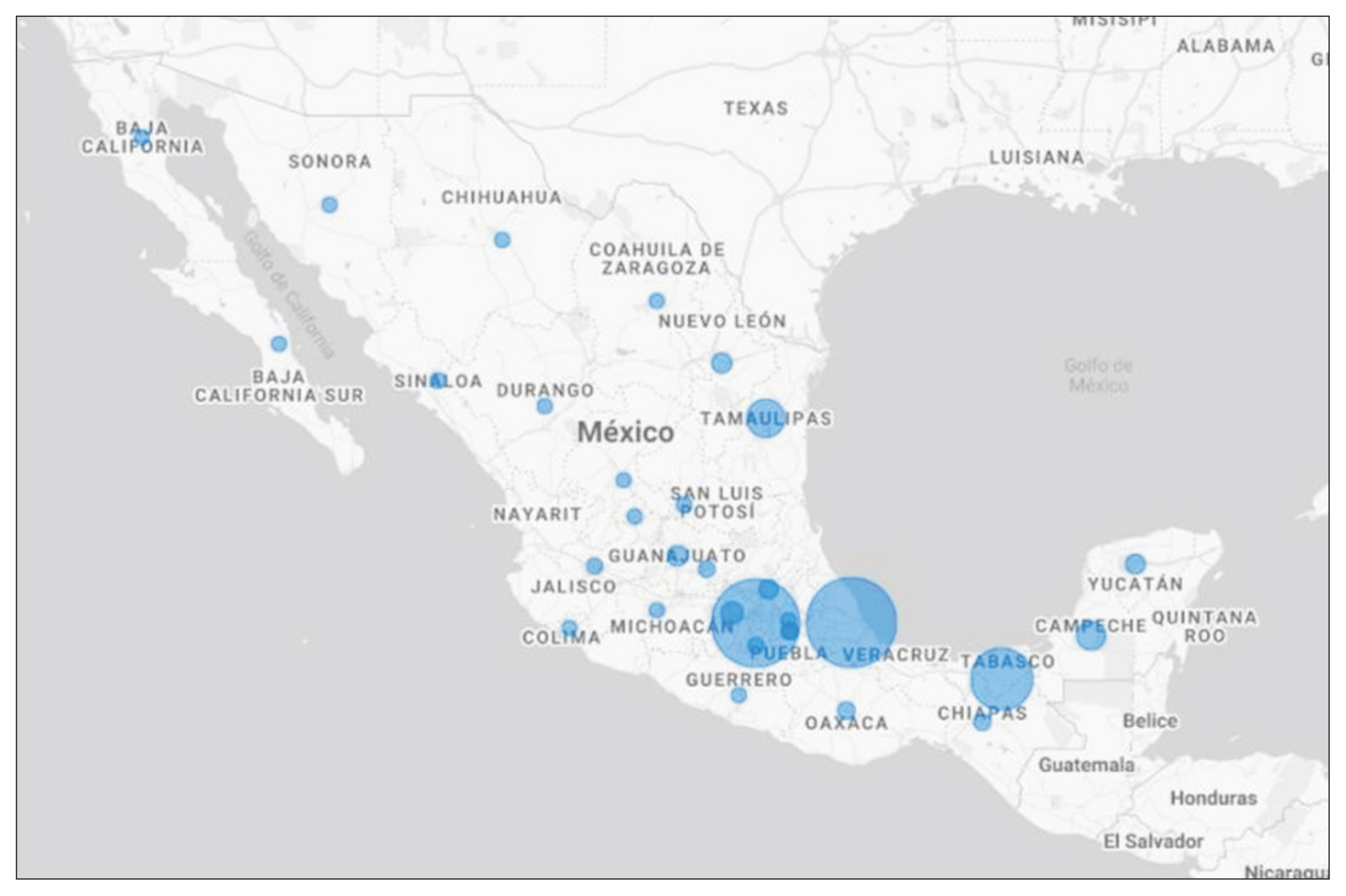
Table 1
Number of participant doctors sorted by specialty and number of answered calls in the remote health program
Table 2
Clinical features of the patients who participated in the program (n = 17,472)
Table 3
Patients referred to a hospital for attention or directly to a specialist
References
1. Garcell HG. COVID-19: a challenge for healthcare professionals. Rev Habanera Cienc Med 2020;19(2):1-4.

2. Beltran-Aroca CM, Gonzalez-Tirado M, Girela-Lopez E. Ethical issues in primary care during the coronavirus (SARS-CoV-2) pandemic. Semergen 2021;47(2):122-30.


3. Cascella M, Rajnik M, Aleem A, Dulebohn SC, Di Napoli R. Features, evaluation, and treatment of coronavirus (COVID-19). Treasure Island (FL): StatPearls Publishing; 2022.

4. Hollander JE, Carr BG. Virtually perfect?: telemedicine for COVID-19. N Engl J Med 2020;382(18):1679-81.


5. Centers for Disease Control and Prevention. Using telehealth to expand access to essential health services during the COVID-19 pandemic [Internet]. Atlanta (GA): Centers for Disease Control and Prevention; 2020 [cited at 2022 Mar 30]. Available from: https://www.cdc.gov/coronavirus/2019-ncov/hcp/telehealth.html

6. Rodziewicz TL, Houseman B, Hipskind JE. Medical error reduction and prevention. Treasure Island (FL): StatPearls Publishing; 2022.

7. American Hospital Association. Fact sheet: telephone [Internet]. Chicago (IL): American Hospital Association; 2019 [cited at 2022 Mar 30]. Available from: https://www.aha.org/system/files/2019-02/fact-sheettelehealth-2-4-19.pdf

8. Sedano-Chiroque FL, Rojas-Miliano C, Vela-Ruiz JM. Perspective on the primary prevention of COVID-19. Rev Fac Med Hum 2020;20(3):494-501.

9. Centro Nacional de Excelencia Tecnologica en Salud (CENETEC). Acerca de CENETEC-Salud [Internet]. Mexico City, Mexico: CENETEC; 2015 [cited at 2022 Mar 30]. Available from: https://www.gob.mx/salud/cenetec

10. Diario Oficial de la Federacion (DOF). PROJECT of the Mexican Official Standard PROY-NOM-036-SSA3-2015, for the regulation of remote medical care [Internet]. Mexico City, Mexico: DOF; 2015 [cited at 2022 Mar 30]. Available from: http://dof.gob.mx/nota_detalle.php?codigo=5420782&fecha=21/12/2015

11. Ipsos Group. Global views on healthcare in 2018 [Internet]. Paris, France: Ipsos Group; 2018 [cited at 2022 Mar 30]. Available from: https://www.ipsos.com/en/global-views-healthcare

12. Diaz de Leon Castaneda C. ICT in the public sector of the health system of Mexico: advances and opportunities. Acta Univ 2020;30:e2650.

13. Petroleos Mexicanos (PEMEX). Report on the health status of PEMEX workers and beneficiaries affected by COVID-19 [Internet]. Mexico City, Mexico: PEMEX; 2020 [cited at 2022 Mar 30]. Available from: https://www.pemex.com/saladeprensa/boletines_nacionales/Paginas/2020-081_nacional.aspx

14. Petroleos Mexicanos (PEMEX). Operational guide for providing medical attention to COVID-19 patients in hospitals. [Internet]. Mexico City, Mexico: PEMEX; 2020 [cited at 2022 Mar 30]. Available from: https://www.pemex.com/servicios/salud/NormatecaServiciosdeSalud/Normateca/DTTO-23110-1-001%20Gu%C3%ADa%20Operativa%20Atenci%C3%B3n%20COVID-19%20Difusi%C3%B3n%20R.pdf

15. Gao YD, Ding M, Dong X, Zhang JJ, Kursat Azkur A, Azkur D, et al. Risk factors for severe and critically ill COVID-19 patients: a review. Allergy 2021;76(2):428-55.



16. World Health Organization. COVID-19 continues to disrupt essential health services in 90% of countries [Internet]. Geneva, Switzerland: World Health Organization; 2021 [cited at 2022 Mar 30]. Available from: https://www.who.int/news/item/23-04-2021-covid-19-continues-to-disrupt-essential-health-services-in-90-of-countries

17. Javanparast S, Windle A, Freeman T, Baum F. Community health worker programs to improve healthcare access and equity: are they only relevant to low- and middle-income countries? Int J Health Policy Manag 2018;7(10):943-54.




18. Babatunde AO, Abdulazeez AO, Adeyemo EA, Uche-Orji CI, Saliyu AA. Telemedicine in low and middle income countries: closing or widening the health inequalities gap. Eur J Environ Public Health 2021;5(2):em0075..

19. Budd J, Miller BS, Manning EM, Lampos V, Zhuang M, Edelstein M, et al. Digital technologies in the public-health response to COVID-19. Nat Med 2020;26(8):1183-92.



20. Kane CK, Gillis K. The use of telemedicine by physicians: still the exception rather than the rule. Health Aff (Millwood) 2018;37:1923-30.


21. Chinese Community Health Plan. COVID-19 telehealth coverage policies [Internet]. San Francisco (CA): Chinese Community Health Plan; 2021 [cited at 2022 Mar 30]. Available from: https://www.cchpca.org/resources/covid-19-telehealth-coverage-policies/


22. Petroleos Mexicanos (PEMEX). Operational information services (SIO)/december population structure. [Internet]. Mexico City, Mexico: PEMEX; 2021 [cited at 2022 Mar 30]. Available from: https://www.pemex.com/servicios/salud/paginas/home.aspx

23. Migongo AW, Charnigo R, Love MM, Kryscio R, Fleming ST, Pearce KA. Factors relating to patient visit time with a physician. Med Decis Making 2012;32:93-104.



24. de la Calle JL, Abejon D, Cid J, del Pozo C, Insausti J, Lopez E. Quality care standards and procedures catalogue in chronic pain units. Rev Soc Esp Dolor 2010;17(2):114-33.

25. Lemus J, Araguesy Oroz V. Medical Audit, a systemic approach [Internet]. Buenos Aires, Argentina: Ediciones Universitarias; 2004 [cited at 2022 Mar 30]. Available from: http://www.medicos-municipales.org.ar/titu51104.htm

26. Baldwin L, Clarke M, Hands L, Knott M, Jones R. The effect of telemedicine on consultation time. J Telemed Telecare 2003;9 (Suppl 1):S71-3.


27. Pan American Health Organization. Framework for the implementation of a telemedicine service [Internet]. Washington (DC): Pan American Health Organization; 2016 [cited at 2022 Mar 30]. Available from: https://iris.paho.org/bitstream/handle/10665.2/28414/9789275119037_eng.pdf

- TOOLS
-
METRICS

-
- 0 Crossref
- Scopus
- 3,458 View
- 190 Download
- Related articles in Healthc Inform Res
-
Path to Advanced Healthcare in the Wake of COVID-192020 April;26(2)